- Tongue Tie
- Transgender and non-binary lactation support
- Sore or Cracked Nipples
- Over/ Under Supply
- Engorgement
- Thrush
- Blocked Ducts and Mastitis
- Pumping
- Useful Links
- Publications by Dr Silberstein
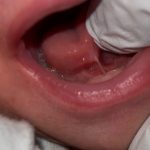
Tongue Tie occurs when tongue movement is restricted by the presence of a short, tight membrane (known as the lingual frenulum) which stretches from the underside of the tongue to the floor of the mouth. This strand of tissue is visible when the tongue is lifted and is a normal part of anatomy. However, when it is short, tight, and inelastic, extends along the underside of the tongue or is attached close to the lower gum it will interfere with the normal movement and function of the tongue and is a tongue-tie. The baby has difficulties building up a good vacuum during the feed as well emptying the breast efficiently due to the malfunction of the tongue. It is more common in boys and around 10-20% of babies will be born with a tongue tie.
Recently the knowledge about Tongue Tie has increased and luckily the number of midwifes, doctors, Health Visitors and nurses who are able to diagnose or at least suspect a tongue tie is growing, although there is still a big room for improvement and it is not standard practise to check or treat them in the hospital after birth.
There are a few ways of classifying tongue ties, we grade them into Grade I-IV or in percent, 25-100%, depending on the location of the frenulum attaching from the underside of the tongue to the gumline or floor of the mouth. Some forms of tongue tie are very easy to diagnose and simple to spot, other variations require skilled assessment as they are often embedded and need to be diagnosed by a professional trained in diagnosing and treating Tongue Ties.
Some signs of Tongue Tie in mums are: painful feeding, cracked nipples, misshapen, white nipples, painful latch and engorged breasts, recurrent blocked ducts, mastitis.
Baby’s symptoms can be: a white membrane visible under tongue when crying, a heart shaped tongue, inability to open their mouths wide, tongue mobility is restricted, slow weight gain, clicking sound during feeds, sucking cheeks in, gulping and spluttering, very windy and colicky, screaming after a feeds, fussy on the breast, sliding off during a feed, needs repositioning, dribbling down the side of the mouth and others, reflux, spitting up.
The criteria for treatment are feeding difficulties. If the mother has received breastfeeding support and correcting latch and positioning don’t have enough effect then surgical treatment as soon as possible is advisable. This will help mothers to continue breastfeeding instead of switching to formula.
Some bottle fed babies also require treatment. Restricted tongues have the inability to build up a vacuum. Those babies often dribble while feeding and are often very unsettled because they swallow a lot of air. Many cough, splutter and choke on the bottle as the limited mobility of the tongue doesn’t allow for managing the milk flow. The milk flows unhindered towards the back of the throat, which leads to choking.
Tongue Ties can have long term consequences. It can lead to difficulties weaning onto chunky foods, as the tongue can’t move the food around the mouth. Many tongue tied babies are being fed finely pureed food and struggle to drink from a cup. Speech problems can occur due to the limited tongue movement. Orthodontic issues due to restricted jaw growth which can lead to overcrowding and crooked teeth. Many adults with untreated tongue ties will report problems with TMJ pain, clicky jaws, snoring and mouthbreathing.
Lip ties: some very severe lip ties can have an influence on breastfeeding but most cases will be resolved by just revising the Tongue Tie. In the UK the official guidelines state that as opposed to Tongue Tie Division there is not enough evidence to support the benefits for breastfeeding and is therefore not performed as a standard procedure.
The tongue tie procedure is usually performed without anaesthetic up to 1 year of age, (varying between services and experience of the practitioner) and is usually very well tolerated. The baby is swaddled and head and shoulders need to be held to minimise movement. The frenulum is cut with sharp, blunt surgical scissors. There should be minimal bleeding and it is encouraged to breastfeed baby straight after that for comfort but also so that the tongue can press down on the wound. Complications such as prolonged bleeding or infections are very rare (1:10000) and most babies recover and heal very well. If the baby is older than 2 months it is permissible to give paracetamol before and after the procedure, it may not be necessary.
Aftercare includes keeping the site very clean, do not let baby suck fingers that haven’t been washed thoroughly with soap, if baby uses a dummy or bottle, make sure it is sterilised.
Massaging the wound several times a day to prevent the regrowth or reattachment of the frenulum can potentially help but there has not been any scientific prove for or against it yet. There are some exercises I show the parents which will encourage tongue movement and need to be done 4-5 times a day for 3-4 weeks. Making sure a deep latch is practised after the procedure is a good way to keep the tongue moving. Unfortunately about 2-4% of the cases will reattach and will have to be re-revised if the symptoms return.

Unfortunately most mothers will experience some degree of pain or discomfort during their breastfeeding journey. Pain is not normal and shouldn’t be accepted. There usually is an underlying reason for it. Often it is the latch that needs improving, sometimes an undiagnosed or untreated tongue tie, occasionally it can be trush, etc. it is a good idea to seek professional help if you experiece nipple pain in order to find the cause and deal with it. Ideally breastfeeding should be painfree and an enjoyable experience for both, mother and baby. If the mother has to endure discomfort she is much more likely to give up breastfeeding well before the recommended duration.
A good attachment means that the nipple is moving against the baby’s soft palate. if a poor, shallow latch is present, the nipple will not be far enough in baby’s mouth and therefore is rubbing against the hard palate. In a lot of cases a Tongue Tie is responsibe for the baby’s inability to open his/her mouth wide enough to manage a good latch and to maintain it for the duration of the feed (baby will often loose the vaccum, slip off the breast or unlatch frequently).
In a lot of cases a flattened, misshapen nipple can be observed, which is a sign that the nipple was compressed by tongue and hard palate.
In case of pain it is always advisable to seek the professional help of a Board Certified Lactation Consultant (IBCLC) or a qualified Breastfeeding Counsellor to find the reason for the pain.
During breastfeeding
- Breastfeed from the intact or less injured breast first as baby will tend to feed more gently on the second side offered
- Trying out different breastfeeding positions to find the most comfortable.
- It is very important to keep emptying the breasts, so if breastfeeding is too painful, keep expressing in order to avoid mastitis and to maintain the milksupply.
After breastfeeding
- Soak nipples in warm saline or use a squirty bottle to soak the nipples, pat them dry gently
- Expressed breastmilk applied to the nipples promotes healing.
- “Moist wound healing” is a concept used in surgical wound healing, apply a medical grade lanolin ointment (e.g. Lansinoh) or a hydrogel dressing (e.g., Multimam, Jelonet, Novogel).
- If you have thrush, follow the saline soak with an antifungal creme (Daktarin)
- If needed, apply an antibiotic ointment (e.g. Bactroban) sparingly after each feed.
Oversupply
Generally it will take 4-6 weeks until the milk supply is established, meaning that supply and demand are just right for the baby. Occasionally women have such an abundant milk supply that the baby struggles to control the flow and starts gagging, spluttering, coughing or clamping down in an attempt to slow the flow. Practising the best possible latch and various positions that let the baby sit more upright will be most helpful. In some cases it can look like an over supply but the underlying reason for engorgement and coughing or gagging can be a Tongue Tie when baby’s tongue is unable to move the milk efficiently to the back of the throat. Inefficient peristaltic and an incomplete seal around the areola can lead to inability to cope with a fast flow.
Undersupply
It requires a professional assessment to establish if there is in fact a low milk supply or if mums have the perception they should have more milk. The fact that breasts don’t leak, soft breasts, frequent feeds, the amount of expressed breast milk or a lack of feeling a let-down does not mean that there is an issue with the milk supply.
Here are a few signs of a low milk supply:
– The baby is being fed on demand (unrestricted and is offered both breasts) and is not gaining weight on breast milk alone
– a lack of wet and dirty nappies
The following things can cause or contribute to a low milk supply:
– Supplementing. Breast milk is made by supply & demand. The more baby feeds, the more milk is being produced. Every time the baby is being given a bottle and the breasts are not emptied the body sends a signal to the brain to produce less.
The same is true for scheduled feeding. The milk supply can decrease if the baby is not allowed to cluster feed to bring the supply up during growth spurts. It is of utmost importance to feed a baby responsively whenever the baby demands.
– Limiting the feed to one breast. This is only a good option for mothers with abundant/ or over supply. Otherwise, this can lead to low milk supply. The same applies to limiting the length of a feed. Timing the feed and taking the baby off the breast prematurely can cause the baby to miss out on the milk with higher fat content that is available to the baby towards the end of the feed.
– Nipple confusion. The use of bottles can confuse the breastfed baby. Babies quickly get used to a teat and the different sucking mechanics required while bottle feeding and can lead to less efficient sucking on the breast.
– Use of dummies. The use of dummies can reduce the time the baby spends on the breast. By giving a dummy it is very possible to miss those first feeding cues and this might lead to longer feeding intervals. This is why we don’t recommend the dummy use for the first 4 weeks or until breastfeeding is fully established.
– Nipple shields. In some cases nipple shields have to be used to successfully breastfeed but should only be used if entirely necessary and weaned off as soon as possible. The latch is never as deep as without a shield and this can lead to decreased milk transfer.
– Sleepy baby. It is normal for newborns to be sleepy, especially when they are jaundiced. It is important to wake baby up for feeds if they don’t do so naturally, every 2 hours in the day and every 4 hours at night in order to establish a good milk supply.
– Health or anatomical problems with baby (including jaundice, tongue tie, etc.) can prevent baby from removing milk adequately from the breast
– Mother’s health (uncontrolled anaemia or hypothyroidism, retained placenta, post-partum haemorrhage…), previous breast surgery/injury, hormonal problems (e.g. PCOS), obesity, medications (contraceptive pill or other medications known to decrease supply), drinking of herbal Teas such as peppermint or sage, or smoking also have the potential to affect milk supply. Some mothers suffer from IGT (Insufficient Glandular Tissue), a condition where the breast does not have enough breast tissue that can produce milk. With good support and a good supplementation plan (if possible with the use of the SNS) it is still possible to have a good breastfeeding experience.
When breasts are engorged, they are very full of milk, and may feel big, hard, heavy and tender. The swelling usually affects both breasts at the same time, and can stretch the nipples so that they are flat. Some women fel hot or even a bit feverish. It is important to feed baby on demand, the more baby feeds, the quicker the engorgement will subside. The baby should empty one side as much as possible and the other breast should be offered afterwards. If the pain has not improved it is possible to handexpress or use a pump to relieve the breasts. It is important to treat engorgement appropriately because it increases the chances of developing a painful inflammation of the breast.
Thrush is a fungal infection on the maternal nipple and breast and can sometimes develop on cracked or injured nipples and in the baby’s mouth. Often there is a history of antibiotic treatment during or around labour or if the newborn was treated at some point. Antibiotics reduce the number of helpful bacteria and allow the candida yeasts to grow.
Symptoms of thrush are a sudden start of breast and/or nipple pain in both breasts after a time of pain free breastfeeding, shiny and/or red nipples, burning sensation in your nipples. The pain can be severe and can last for up to 1 hour after every breastfeed.
Symptoms of thrush in the baby are creamy white patches in the baby’s mouth, on the tongue and may be far back or in the cheeks which don’t rub off. Baby’s tongue/lips may have a white gloss.
Thrush can be passed between mother and baby, therefore it is important to treat both. Extra hygiene measures should be put in place to eradicate thrush completely (such as daily, towel changes, changing breast pads after each feed, changing the bra every day and washing it on a high temperature and washing your hands frequently with soap and warm water). It is a good idea to reduce the sugar levels in the mother’s diet. It is a good idea to take a course of probiotics to support the growth of the healthy gut flora.
A blocked duct is an area of the breast where the milk flow is obstructed. This blockage could be in the nipple pore, where this shows as a Milk Blister (bleb) or further inside the breast tissue in the ductal system, where it would manifest in a hard lump that might feel swollen, red, painful and hot. occasionally there is no lump but only tenderness and redness. Blocked ducts will typically feel better after feeding.
There are a wide variety of pumps available on the market: manual pumps, single and double electric, hospital grade electric pumps, hands-free pumps. The best model will depend on the individual’s requirements.
Most electric pumps on the market are ‘open systems’ and are not designed for use for multiple users as there is a possibility for germs and fungus to grow inside the pump. ‘Closed system’ pumps are also known as ‘hospital grade’, which can be, after thorough sterilisation, used by multiple users. The use of a second hand pump (unless it is a hospital grade model) is discouraged due to the contamination risk.
When using an electric breast pump, it is very important to follow the assembly instructions carefully, as leaving a part out or attaching it incorrectly could lead to malfunctioning or leakage from the pump. Most electric pumps are made up of a flange (or two flanges in the case of a double pump), valves (usually made from silicone), backflow protectors, tubing which connects the bottle with the pump, and the collection bottles.
It is crucial to ensure the flanges fit properly. The nipple should fit snugly inside the flange funnel; there shouldn’t be any rubbing (as this would indicate the flange is too small) and the areola should not get sucked in (which would indicate that the flange is too large). Many companies supply a standard flange size of 24mm, and some companies produce size 21mm-36mm to cater for various nipple sizes. If you are unsure of the correct size for you, speak to a breastfeeding specialist.
Step by step: using a breast pump
Before using a pump, you should always wash your hands with soap and warm water. Be sure not to touch the parts that come into contact with milk in order to avoid contamination.
For good milk output, it is helpful to be sitting as comfortably as possible, and to have a drink and a snack ready. Being close to your baby, having a muslin that smells of them, or even looking at a photo or video of your baby will help with the milk to flow.
It can be helpful to apply a warm compress to the breast for a few minutes before pumping as this enhances circulation, and then to massage your breasts to encourage the let-down reflex, massaging the whole breast in a circular motion, using your fingertips as well as stroking motions with your palm or the flat of your hand.
Place your nipple in the centre of the flange and turn the pump on. A lot of pumps have a 2-phase technology, whereby the pumping cycle starts with short, light sucks to trigger the let-down reflex, followed by slower and stronger sucks. If you want to control the settings manually, at the start of a session, the vacuum needs to be set on low, with the cycles set on high. Once the milk starts to flow, the cycle speed needs to be decreased and the suction strength should be increased to a comfortable level, which is strong enough to get the milk to flow, but not too strong as this can cause pain, which inhibits milk flow.
The volumes a mother can express vary considerably depending on the age of the baby, maternal milk supply, pumping frequency and the length of the pumping session, and whether she is exclusively pumping or pumping after a breastfeed. How long it takes for a mother to experience the let-down reflex can vary greatly between mothers, and it is not a good idea to compare yourself with other mums as this can lead to unfounded feelings of inadequacy. Most of the available milk will be removed within 15-20 minutes, although it’s important to be aware that lactating breasts are never completely empty. If the aim is to increase supply, it is helpful to pump for a few minutes after the milk has stopped flowing.
After you have finished expressing, label the bottle with the date and time of the expressing session, and place it in the fridge (or freezer if it needs to be stored for longer) until you need the milk.
Recommended storage details:
- Room temperature (77°F/25°C) for up to 6 hours
- In main part of fridge (below 4°C) for up to 5 days (up to 8 days according to some sources)
- Warmer fridge (5°C—10°C) for 3 days
- Freezer (approx. –18°C) for 6 months
- Previously frozen/thawed milk 12 – 24 hours in fridge
(https://abm.me.uk/breastfeeding-information/expressing-breast-milk/)
Reasons for pumping:
It is not recommended to use a pump before birth, but it can be helpful to start hand expressing milk from 36 weeks pregnancy (more information: https://www.llli.org/the-benefits-of-antenatal-colostrum-harvesting/) in preparation for the baby’s arrival.
After the baby’s birth, there is no need to pump if they are feeding well from the breast and if the milk supply is sufficient. Pumping in the early weeks should only be done if there is a need, such as:
- low milk supply.
- nipple injuries that prevent the baby from feeding directly from the breast.
- separation of mum and baby
- if the baby has special needs (such as cleft lip or palate, Down’s Syndrome, or a cardiac condition).
- if the baby was born prematurely (or small for gestational age).
- if the baby cannot latch onto the breast.
Once breast milk supply has been established, which is around 4-6 weeks, some mums like to pump to build up a freezer stash, for when they go back to work, so they can introduce a bottle, or for example in case there is a medical reason which means they need to stop breastfeeding – although this is rare. (Please always double-check with a lactation consultant).
What to do if pumping is painful?
Pumping should not be uncomfortable. Pain while pumping can be caused by an ill-fitting flange, which is either too small and chafing the skin of your nipples, or too big and pulling your areola into the funnel of the flange. Please ask a breastfeeding specialist to check the fit of the flange if you are experiencing pain. If the pain does not settle despite a correct flange size, it is advisable to seek help from a specialist.
How to increase the milk yield when pumping:
- The main way to increase the milk supply is to ensure frequent emptying of both breast (at least 8 times in 24 hours)
- Ensure a good flange fit
- Replace pump parts if the pump is not new. The silicone valves and membranes can get brittle from repeated sterilisation and prolonged use
- Prepare the breast by applying warm flannels and massaging the breasts before pumping
- Find the right pump setting for you (as high as possible without being uncomfortable)
- Find the right time of day (milk flow is often better in the morning and decreases towards the evening)
- Pump near the baby if possible or while breastfeeding on the other breast
- Make sure you are as comfortable as possible and try to relax while pumping
- Try not to look at the bottles and how much milk is collecting as this can cause anxiety and reduce the flow
- Double pumping (both breasts simultaneously) gives a better milk yield than single pumping, it is also time saving
- Hands on pumping: breast massage and breast compressions while pumping can increase the flow
- Taking a break for a few minutes after the first let-down reflex has stopped, and starting again, can help to catch a second let-down.
How often do I need to pump?
Breast milk is produced on a supply and demand basis. Thorough and frequent emptying of the breast will help to increase your levels of prolactin, the hormone responsible for milk production.
How often a mother needs to pump depends a lot on the situation and the reason why pumping is necessary. If a baby is unable to breastfeed, it is recommended that the pumping frequency mimics a baby’s feeding pattern, which is at least every 3 hours, 8 times in 24 hours (ideally 2-hourly in the day and 4-hourly at night). It is crucial not to let the gaps between the pumping sessions get too long, in order to ensure plenty of breast stimulation, sufficient expressed milk to feed the baby, and to avoid breast engorgement or a drop in milk supply.
If the baby is also breastfeeding, some of the breastfeeds can be replaced by expressing.
If a baby is breastfed but not efficient at emptying the breast, the pump can be used after a feed in order to maintain milk supply and so the baby can be supplemented with expressed milk. In some cases (for example: excessive weight loss in the baby, tongue-tie, prematurity) a feeding regime might have to be put in place, whereby every breastfeed is followed by a pumping session and a top-up of expressed milk (or formula). This is called ‘triple feeding’ and is mostly a temporary measure to ensure good weight gain.
- https://toxnet.nlm.nih.gov/newtoxnet/lactmed.htm
- https://www.breastfeedingnetwork.org.uk/about-us/
- http://www.breastfeedinginpublic.co.uk/
- http://publicbreastfeedingawarenessproject.com/
- http://kellymom.com/
- https://www.breastfeedingnetwork.org.uk/
- https://www.laleche.org.uk/
- https://www.nct.org.uk/
- http://www.nhs.uk/conditions/pregnancy-and-baby/Pages/benefits-breastfeeding.aspx
- http://www.breastfeedinginc.ca/index.php
- http://www.uhs.nhs.uk/OurServices/Childhealth/Tonguetie/Tonguetie.aspx
- https://www.nice.org.uk/guidance/IPG149
- http://www.tongue-tie.org.uk/tongue-tie-information.html
- Tsippy Kraus Antenatal classes and Doula services: http://www.theswissmethod.co.uk/
-
http://www.private-gp-in-london.co.uk/medico-legal-reports-expert-witness Dr. Martin Harris, Private GP, Circumcisions, Bris Milas and medico legal reports www.circumcisionlondon.co.u
- Carl Irwing, Doctor of Chiropractic & Clinic Director https://www.spinelab.co.uk/
- Dr. Ella Rachamim, first aid training for parents and professionals http://www.bereadytoparent.com/
- Stacey Zimmels, feeding and speech therapy https://www.feedeatspeak.co.uk/









